At most healthcare organizations, credentialing is treated like a cost center.
It’s something you have to do.
Something you staff.
Something you try to keep compliant.
And if everything is working, it stays
in the background.
But here’s the problem.
When credentialing isn’t working, it doesn’t just create operational friction.
It delays revenue.
This is where most organizations get stuck
We talk to a lot of health systems that know something is off.
Providerstake too long to get activated.
Teams are constantly chasing information.
No one has a clear view of where things stand.
But when you ask this simple question, “How long does it take you to get a provider fully billable?”
Most organizations don’t have a clear answer. Not because they aren’t trying. Because the system isn’t built to give them one.
Credentialing isn’t broken. It’s underbuilt.
Most attempts to fix credentialing focus on the surface.
Add a tool.
Standardize a workflow.
Push teams to move faster.
That might improve things incrementally.
But it doesn’t solve the underlying issue.
Credentialing isn’t just a process.
It’s infrastructure.
And if the infrastructure isn’t there, performance will always lag behind expectations.
What we actually see in the market
When you step back, there’s a clear pattern.
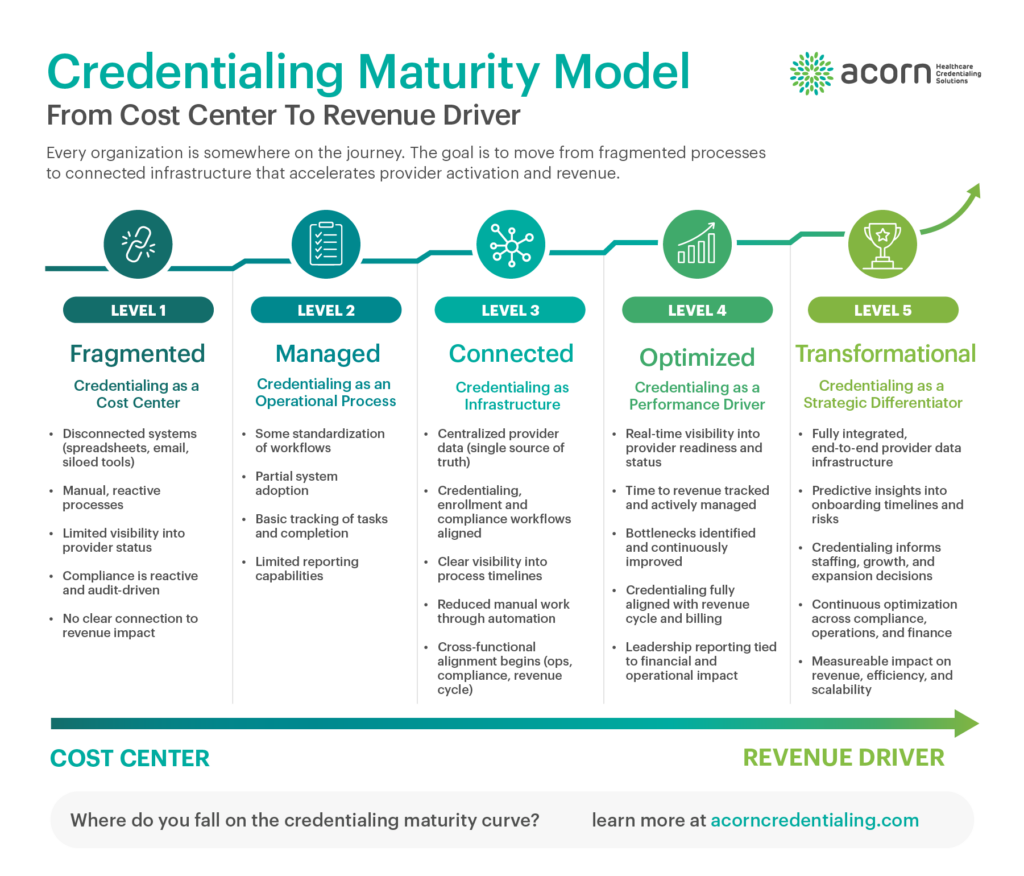
Organizations fall into a progression—whether they realize it or not.
At the low end, everything is fragmented
Work lives in spreadsheets and inboxes.
Teams operate in silos.
Information is inconsistent.
Delays are constant.
You know it’s slow, but you can’t pinpoint why.
And you definitely can’t quantify what it’s costing you.
Then things start to feel more “managed”
There’s more structure. Some standardization.
But systems still don’t talk to each other.
Teams still operate separately.
Work gets done, but it’s heavier than it should be.
The shift happens when things become connected
This is where organizations start to turn a corner.
Provider data is centralized.
Credentialing, enrollment, and compliance begin to align.
For the first time, you can actually see what’s happening.
And once you can see it, you can start to improve it.
From there, performance becomes intentional
Now you’re not just managing work.
You’re managing outcomes.
You’re tracking time to revenue.
You’re identifying bottlenecks.
You’re reducing delays in a way that actually shows up financially.
And at the highest level, credentialing changes role entirely
It stops being a function you manage.
It becomes part of how the organization operates.
It informs hiring.
Expansion.
Growth decisions.
At that point, it’s not a cost center anymore. It’s an asset.
What actually drives that shift
Moving from one stage to the next isn’t about working harder.
It comes down to a few fundamental changes.
You need visibility into what’s actually happening.
You need systems that are connected, not layered on top of each other.
And you need to measure credentialing based on outcomes, not just completion.
Without those three things, progress stalls.
Why this matters more for critical access hospitals
For larger systems, inefficiency is expensive.
For critical access hospitals, it’s a real constraint.
You don’t have excess capacity.
You don’t have margin for delay.
If a provider isn’t credentialed and enrolled, you feel it immediately.
That’s why this conversation matters.
Not because credentialing needs to be “better.”
But because it has a direct impact on whether revenue shows up when it should.
The bottom line
Most organizations think they have a credentialing process.
What they don’t have is a system that’s built to perform.
And that’s the difference.
Between something that gets done
and something that actually drives revenue.
Where do you fall on the credentialing maturity curve?
For more information Contact us or Book a Demo