Health Insurance Payers
Solution Features
Eliminate functionality issues that cost time and money, and expose you to unnecessary risk. Acorn does the work of monitoring licensing databases and verifying provider information for you.
Auto Update and Verify State Licenses
In typical environments you run reports, notify providers, and manually verify each provider when they are renewed. With Acorn, this process is fully automated. It saves valuable time by automatically verifying and updating provider credentials in the system, especially for payers that handle a large number of provider credential verifications.
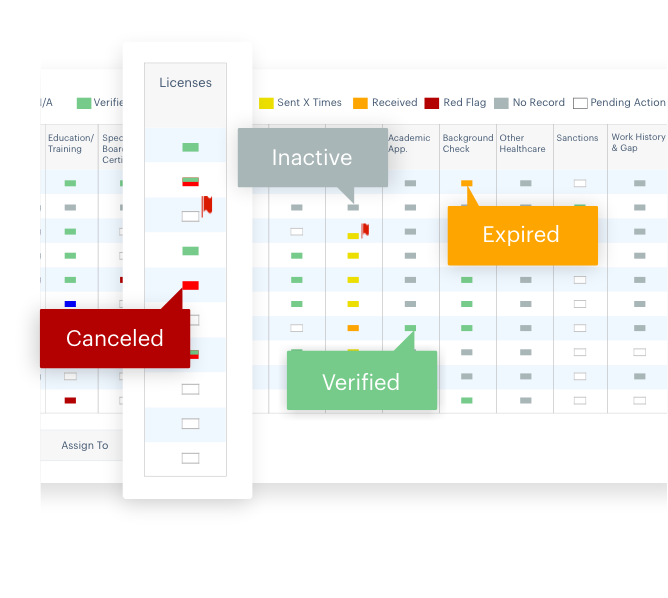
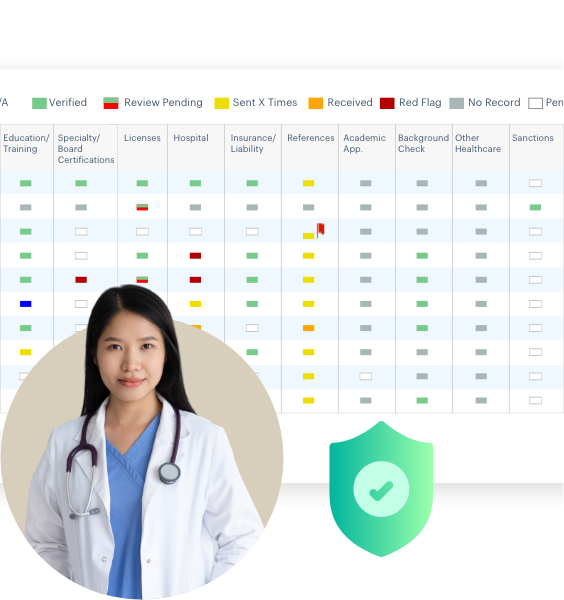
Auto Update and
Verify DEA
DEA registrations are renewed every three years and the renewal date is directly correlated to the date a provider’s registration was first issued. The automatic update and verification feature in Acorn saves time in this process, as well as helping to ensure application deadlines are met. For payers that manage large numbers of providers and their credentials, the Acorn system’s automation streamlines this process significantly.
SAM Sanction Checks
The System for Awards Management (SAM) includes the excluded parties list system (EPLS) which is another source for provider sanctions. The Acorn system checks all providers against the SAM database on a daily basis and users are alerted on the Acorn dashboard if any of their providers are named in this database. The user can then verify the information within the system and bring back the report to verify.
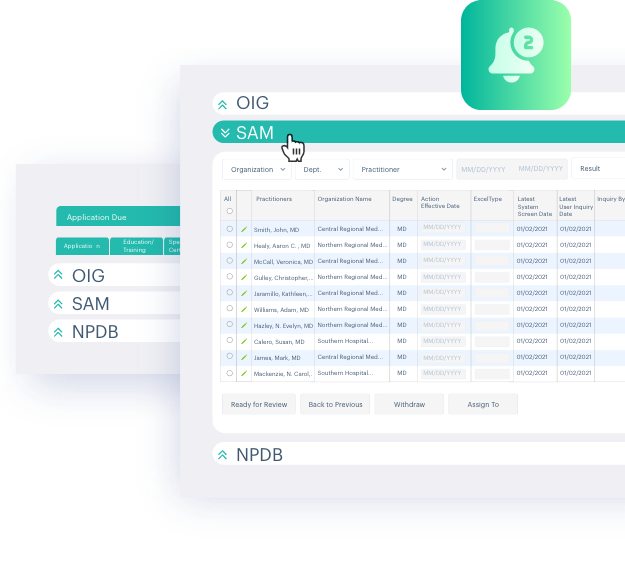
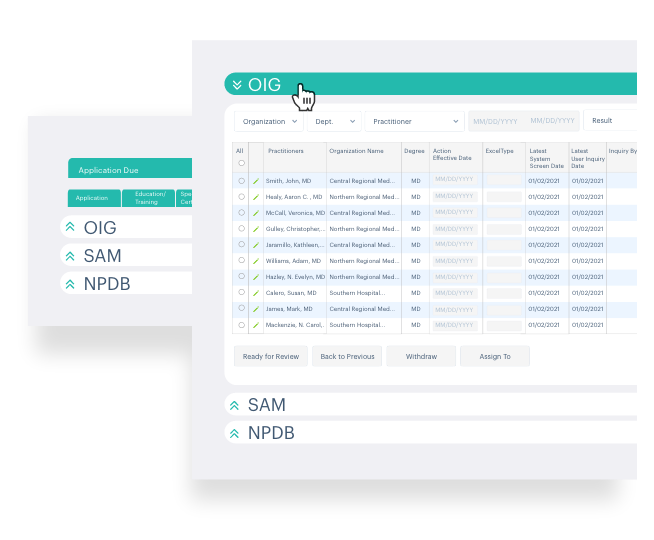
OIG Sanction Checks
The Office of the Inspector General puts out monthly reports of providers with new sanctions. Acorn automatically checks each provider in the system monthly and alerts users on the dashboard of providers that have new sanctions with the OIG.
Mobile Scanner
Scan and upload documents quickly and easily with your mobile phone. And because your phone goes almost everywhere you go, Acorn’s scanning app can also go places physical scanners cannot.















